Aug 10
The Dirty Truth About Sluicing Part 1
A Transformation, not an Obsolescence
It started with a smell. Barely noticeable at first—just part of the background noise in a busy aged care home. But soon, residents became unwell, staff were overwhelmed, and the audit file was pulled out of the drawer. The cause? Outdated and inconsistent waste-handling practices based on traditional sluicing.
In too many New Zealand aged care facilities, sluicing remains the default method for managing human waste. It is regarded as “just the way things are done.” However, it is also a recognised health and safety hazard, an infection risk, and an increasing compliance liability.
This blog is not about eliminating sluicing, but rather gaining a better understanding of the process and the changes implemented due to environmental and infection prevention concerns.
In too many New Zealand aged care facilities, sluicing remains the default method for managing human waste. It is regarded as “just the way things are done.” However, it is also a recognised health and safety hazard, an infection risk, and an increasing compliance liability.
This blog is not about eliminating sluicing, but rather gaining a better understanding of the process and the changes implemented due to environmental and infection prevention concerns.
The Enduring Role of Sluicing in Healthcare
The process of sluicing in healthcare, especially in aged care facilities, is not a practice that has become obsolete. Instead, it has undergone a significant transformation, evolving from basic manual waste disposal to a highly advanced and automated system. This change has been driven by the need for strict infection control and, increasingly, environmental sustainability. Modern sluice rooms, with their state-of-the-art equipment and carefully managed protocols, play a vital role in preventing healthcare-associated infections (HAIs) and maintaining high hygiene standards in aged care facilities and hospitals around the world.
The modern understanding of sluicing extends beyond simply disposing of waste. It now includes a comprehensive "sluice room management” concept that involves precise design, innovative technology, efficient workflow practices, and thorough staff training. This approach reflects a deeper, more refined understanding of infection pathways, recognising that effective infection control requires managing the entire micro-
The modern understanding of sluicing extends beyond simply disposing of waste. It now includes a comprehensive "sluice room management” concept that involves precise design, innovative technology, efficient workflow practices, and thorough staff training. This approach reflects a deeper, more refined understanding of infection pathways, recognising that effective infection control requires managing the entire micro-
environment where contaminated materials are handled. From enhancing air quality and choosing suitable surface materials to ongoing staff education, the sluice room is now seen as a vital, interconnected part of overall patient and staff safety, rather than just an isolated task. This represents a systemic, integrated approach to preventing infections, with the sluice room acting as a proactive control point within the healthcare system.

Defining Sluicing in Healthcare
A sluice room, frequently referred to as a dirty utility room, is a designated, controlled space within healthcare such as hospitals, aged care facilities, and other care establishments. Its primary purpose is the safe and hygienic disposal of human waste products, including urine, vomit, and faecal matter. Beyond disposal, these rooms are also vital for the disinfection and safe handling of associated contaminated items, such as bedpans, vomit bowls, and certain medical equipment. The core emphasis of a sluice room lies in its vital function in preventing cross-infection and maintaining stringent hygiene standards throughout the healthcare setting.
The function of a sluice room is dual: it is used for waste disposal and for disinfecting associated items. Although often seen solely as a waste disposal area, healthcare guidelines and industry descriptions consistently highlight the vital role of disinfection and preparation for reuse. This dual purpose is essential to effective infection control, as
The function of a sluice room is dual: it is used for waste disposal and for disinfecting associated items. Although often seen solely as a waste disposal area, healthcare guidelines and industry descriptions consistently highlight the vital role of disinfection and preparation for reuse. This dual purpose is essential to effective infection control, as
it directly tackles the main issue of healthcare waste: it is not just inert refuse but a potent carrier of pathogens. The disinfection process, whether for reusable items or the room itself, is essential to break the chain of infection. That is why specialised equipment, such as bedpan washer-disinfectors, forms an essential part of modern sluice rooms, since they are designed to do both thorough cleaning and thermal disinfection, making sure items are not only clean but safe for reuse. This complete approach turns what might be viewed as a "dirty" zone into a vital point of control where contamination is actively eliminated and managed, rather than merely contained. It marks a significant shift from older, simpler waste handling methods and shows a better understanding of how infection spreads and how to prevent it.
Why Sluicing Was Used Historically
The historical context of healthcare hygiene highlights a strong need for dedicated sluicing practices. In the early 1800s, hospitals were often criticised as "disease-producing incubators" or "houses of death" due to a severe lack of understanding about hygiene. Conditions were appalling, with many sick and dying patients in wards without proper ventilation or access to clean water. A shocking lack of routine handwashing among doctors persisted until the mid-1800s, directly helping spread diseases between patients. During this period, the popular "miasma concept"—the idea that diseases were caused by inhaling polluted air—clashed heavily with emerging germ theories, which faced fierce opposition until the early 20th century.
Amidst these dire conditions, the emergence of basic sluice sinks marked an early step towards managing infectious waste more hygienically than previous insanitary methods. These early sluice sinks, sometimes called disposal units or slop hoppers, were designed for use in hospitals, nursing homes, and GP surgeries to enable the hygienic disposal of clinical waste, such as the contents of vomit bowls, drainage bags, bedpans, and urine bottles. Although similar in appearance and operation to toilets, their key difference was to keep toilet and waste disposal facilities separate, a measure considered "essential for reducing the risk of cross-contamination and halting the spread of infectious diseases".
Amidst these dire conditions, the emergence of basic sluice sinks marked an early step towards managing infectious waste more hygienically than previous insanitary methods. These early sluice sinks, sometimes called disposal units or slop hoppers, were designed for use in hospitals, nursing homes, and GP surgeries to enable the hygienic disposal of clinical waste, such as the contents of vomit bowls, drainage bags, bedpans, and urine bottles. Although similar in appearance and operation to toilets, their key difference was to keep toilet and waste disposal facilities separate, a measure considered "essential for reducing the risk of cross-contamination and halting the spread of infectious diseases".

The development of "cleanliness" from a cultural practice to a scientific necessity marks a significant chapter in history. Early physical cleansing was often driven by religious motives, with handwashing serving as part of religious and magical rituals for centuries. Later, there was resistance to the scientific understanding of handwashing for disinfection, championed by figures like Maimonides in the 12th century and Ignáz Semmelweis in the 19th century. The earliest use of designated waste disposal areas, such as simple sluices, was likely motivated more by practical concerns like tidiness, odour control, or a general sense of "cleanliness" rather than a clear awareness of microbial transmission. The gradual acceptance of germ theory in the early 20th century suggests that sluicing was originally a practical solution for managing waste, which later became a key, evidence-based infection control practice. This evolution illustrates the long path from basic sanitation to modern infection prevention, shaped by societal and scientific advances.
Furthermore, the separation of sluice sinks from general toilets, even in their simplest form, marks an early recognition of the importance of segregation for infection control. This was a vital step away from simply flushing all waste down any drain to establishing a dedicated, controlled pathway for potentially infectious materials. This early concept of segregation directly led to the "dirty in, clean out" workflow and the careful separation of clean and dirty areas within modern sluice rooms. This seemingly simple design choice was a key early step in creating dedicated infection control infrastructure within healthcare settings. It provided the conceptual and practical foundation for the complex, multi-purpose sluice rooms seen today, showing that the core idea of isolating and handling hazardous waste has deep historical roots and has been progressively refined over time. Historically, manual methods were standard for cleaning bedpans, and the high risks of infection were not always fully acknowledged or addressed, even into the 21st century, with reports indicating up to 50% of bedpans worldwide were still being emptied and cleaned manually by healthcare workers. This ongoing practice, despite its hazards, highlighted the urgent need for automated solutions.
Furthermore, the separation of sluice sinks from general toilets, even in their simplest form, marks an early recognition of the importance of segregation for infection control. This was a vital step away from simply flushing all waste down any drain to establishing a dedicated, controlled pathway for potentially infectious materials. This early concept of segregation directly led to the "dirty in, clean out" workflow and the careful separation of clean and dirty areas within modern sluice rooms. This seemingly simple design choice was a key early step in creating dedicated infection control infrastructure within healthcare settings. It provided the conceptual and practical foundation for the complex, multi-purpose sluice rooms seen today, showing that the core idea of isolating and handling hazardous waste has deep historical roots and has been progressively refined over time. Historically, manual methods were standard for cleaning bedpans, and the high risks of infection were not always fully acknowledged or addressed, even into the 21st century, with reports indicating up to 50% of bedpans worldwide were still being emptied and cleaned manually by healthcare workers. This ongoing practice, despite its hazards, highlighted the urgent need for automated solutions.
The Evolution of Sluicing: From Manual to Automated
The transition from manual waste handling to advanced automated systems in healthcare settings marks an essential milestone in infection control. Traditional manual methods posed significant and inherent risks, such as direct contact with human waste, ineffective manual disinfection, and a high likelihood of cross-contamination, which could lead to healthcare-associated infections (HAIs) for both patients and staff. Manual bedpan cleaning and the use of spray wands are now explicitly discouraged due to their increased infection risk. The risks to caregivers from splashes and aerosols during manual cleaning of bedpans and urine bottles, or when emptying waste, were also substantial, potentially resulting in care worker illness or cross-infection with patients. Even when disinfection was carried out, manual chemical disinfection methods were not considered reliable for treating waste due to variable results and the potential to generate hazardous waste.
These inherent dangers, combined with ongoing advancements in technology and a deeper scientific understanding of microbiology and infection pathways, drove the widespread move towards automated solutions. Modern equipment, such as hospital macerators, is seen as a highly hygienic waste disposal method, breaking down medical pulp products and their contents into a fine slurry before flushing, which greatly reduces human contact. Similarly, bedpan washer-disinfectors automate the cleaning and disinfection of reusable waste containers, effectively sanitising items that come into direct contact with patients and thus lowering the risk of HAIs.
The main driver behind this automation was the considerable risk to healthcare staff from manual waste handling. The ongoing focus on reducing human contact and adopting hands-free technology in modern equipment directly tackles occupational health and safety issues for healthcare workers. This not only protects staff from illness but also potentially decreases staff absenteeism, boosts morale, and markedly enhances overall efficiency by freeing up valuable time from tedious, unpleasant, and risky manual tasks. The point that nurses' time could be "wasted" due to inadequate procedures highlights the operational necessity alongside the clinical one. The continued global prevalence of manual bedpan cleaning, despite known dangers, further underscores a persistent challenge that automation directly addresses and alleviates.
Beyond visible contamination, the shift to automation also addresses the "hidden" risks of manual processes. Manual cleaning often creates "splashes and aerosols," and manual disinfection may fail to eliminate "pathogens that you can't see." This underscores a deeper, more advanced understanding of how microorganisms are transmitted. It's not just about achieving visible cleanliness but about removing microscopic threats that can become airborne, land on surfaces, or stay in the environment. Recognising the sluice room as a potential "centre for cross-transmission" if not managed properly shows that even if gross waste appears to be "gone," the environment can still be dangerously contaminated without proper automated disinfection. This highlights the limitations of human perception and manual efforts in achieving thorough microbial control, making automation essential for effective infection prevention. The move from manual to automated sluicing is a clear response to a more sophisticated scientific view of infection pathways. It marks a crucial shift from basic "cleaning" to proven "disinfection," recognising that proper infection control requires technologies capable of dealing with invisible threats and preventing widespread environmental contamination, thereby raising overall hygiene standards in healthcare.
These inherent dangers, combined with ongoing advancements in technology and a deeper scientific understanding of microbiology and infection pathways, drove the widespread move towards automated solutions. Modern equipment, such as hospital macerators, is seen as a highly hygienic waste disposal method, breaking down medical pulp products and their contents into a fine slurry before flushing, which greatly reduces human contact. Similarly, bedpan washer-disinfectors automate the cleaning and disinfection of reusable waste containers, effectively sanitising items that come into direct contact with patients and thus lowering the risk of HAIs.
The main driver behind this automation was the considerable risk to healthcare staff from manual waste handling. The ongoing focus on reducing human contact and adopting hands-free technology in modern equipment directly tackles occupational health and safety issues for healthcare workers. This not only protects staff from illness but also potentially decreases staff absenteeism, boosts morale, and markedly enhances overall efficiency by freeing up valuable time from tedious, unpleasant, and risky manual tasks. The point that nurses' time could be "wasted" due to inadequate procedures highlights the operational necessity alongside the clinical one. The continued global prevalence of manual bedpan cleaning, despite known dangers, further underscores a persistent challenge that automation directly addresses and alleviates.
Beyond visible contamination, the shift to automation also addresses the "hidden" risks of manual processes. Manual cleaning often creates "splashes and aerosols," and manual disinfection may fail to eliminate "pathogens that you can't see." This underscores a deeper, more advanced understanding of how microorganisms are transmitted. It's not just about achieving visible cleanliness but about removing microscopic threats that can become airborne, land on surfaces, or stay in the environment. Recognising the sluice room as a potential "centre for cross-transmission" if not managed properly shows that even if gross waste appears to be "gone," the environment can still be dangerously contaminated without proper automated disinfection. This highlights the limitations of human perception and manual efforts in achieving thorough microbial control, making automation essential for effective infection prevention. The move from manual to automated sluicing is a clear response to a more sophisticated scientific view of infection pathways. It marks a crucial shift from basic "cleaning" to proven "disinfection," recognising that proper infection control requires technologies capable of dealing with invisible threats and preventing widespread environmental contamination, thereby raising overall hygiene standards in healthcare.
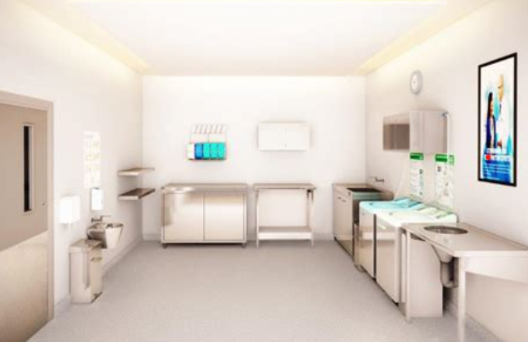
Sluicing in Modern Healthcare: A Vital, Evolved Process
Is Sluicing Still Used?
Sluicing is unequivocally still a vital and continuously evolving process in modern healthcare, particularly within aged care facilities. Sluice rooms are in constant operation, often "24 hours a day, 7 days a week," underscoring their continuous and critical importance for infection control. These designated areas remain essential for maintaining hygiene standards and preventing the spread of infections across hospitals, aged care facilities, and care homes globally. Their primary purpose continues to be the management of biological waste and contaminated items, supporting essential processes like emptying bedpans, rinsing urinals, and cleaning reusable medical ware.
Watch out for the second part of this blog, which explores the modern sluice room, looking at best practices, technologies, and the regulatory environment.
Seek further information from the HUB, ask EVE, our multilingual “bot”, or contact our friendly team at support@infectioncontrol.care for more details.
We are on Facebook and LinkedIn. Like us, follow and share.
Take advantage of our expertise in IPC. See the HUB for policies, resources and courses relating to this very important subject. Ask EVE for a quick answer to your question.
Watch out for the second part of this blog, which explores the modern sluice room, looking at best practices, technologies, and the regulatory environment.
Seek further information from the HUB, ask EVE, our multilingual “bot”, or contact our friendly team at support@infectioncontrol.care for more details.
We are on Facebook and LinkedIn. Like us, follow and share.
Take advantage of our expertise in IPC. See the HUB for policies, resources and courses relating to this very important subject. Ask EVE for a quick answer to your question.
Lyndon Forrest
Managing Director | CEO
Lyndon is the Managing Director of Infection Prevention Services (IPS), bringing over 30 years' experience supporting aged care providers across Australia and New Zealand.
With a background spanning outbreak response, compliance, and infection risk management — alongside hands-on experience leading teams, managing multi-site operations, and navigating business turnaround — he understands both the clinical and organisational pressures aged care providers face. Lyndon holds a Master of Commerce (Industrial Relations), and applies that foundation to the people, process, and growth challenges that come with running a complex healthcare services business.
He is passionate about building the systems and capability that make infection prevention sustainable — not just compliant — and about helping organisations grow their confidence alongside their practice.
Lyndon's focus is straightforward: strengthen operations, develop the right people, and drive proactive infection prevention strategies that protect residents, staff, and communities for the long term.
Lyndon is the Managing Director of Infection Prevention Services (IPS), bringing over 30 years' experience supporting aged care providers across Australia and New Zealand.
With a background spanning outbreak response, compliance, and infection risk management — alongside hands-on experience leading teams, managing multi-site operations, and navigating business turnaround — he understands both the clinical and organisational pressures aged care providers face. Lyndon holds a Master of Commerce (Industrial Relations), and applies that foundation to the people, process, and growth challenges that come with running a complex healthcare services business.
He is passionate about building the systems and capability that make infection prevention sustainable — not just compliant — and about helping organisations grow their confidence alongside their practice.
Lyndon's focus is straightforward: strengthen operations, develop the right people, and drive proactive infection prevention strategies that protect residents, staff, and communities for the long term.
Erica Callaghan
Marketing Manager
Erica Callaghan is a dedicated professional with a rich background in agriculture and nutrient management. Growing up on her family's farm in Mid Canterbury, she developed a deep passion for farming. She currently resides on her partner's arable property in South Canterbury.
In 2017, Erica joined the Farm Sustainability team, focusing on nutrient management and environmental stewardship. In February 2024, she became the Manager of Marketing and Sales at Bug Control New Zealand - Infection Prevention Services, where her passion now includes improving infection prevention outcomes.
Outside of work, Erica loves cooking and traveling, often combining her culinary interests with her explorations in Italy and Vietnam. She enjoys entertaining family and friends and remains actively involved in farm activities, especially during harvest season.
Erica Callaghan is a dedicated professional with a rich background in agriculture and nutrient management. Growing up on her family's farm in Mid Canterbury, she developed a deep passion for farming. She currently resides on her partner's arable property in South Canterbury.
In 2017, Erica joined the Farm Sustainability team, focusing on nutrient management and environmental stewardship. In February 2024, she became the Manager of Marketing and Sales at Bug Control New Zealand - Infection Prevention Services, where her passion now includes improving infection prevention outcomes.
Outside of work, Erica loves cooking and traveling, often combining her culinary interests with her explorations in Italy and Vietnam. She enjoys entertaining family and friends and remains actively involved in farm activities, especially during harvest season.
Toni Sherriff
Clinical Nurse Specialist
Toni is a Registered Nurse with extensive experience in Infection Prevention and Control. Her career began as a kitchen hand and caregiver in Aged Care facilities, followed by earning a Bachelor of Nursing.
Toni has significant experience, having worked in Brisbane’s Infectious Diseases ward before returning home to New Zealand, where she continued her career as a Clinical Nurse Specialist in Infection Prevention and Control within Te Whatu Ora (Health NZ).
Toni brings her expertise and dedication to our team, which is instrumental in providing top-tier infection prevention solutions to our clients.
Toni is a Registered Nurse with extensive experience in Infection Prevention and Control. Her career began as a kitchen hand and caregiver in Aged Care facilities, followed by earning a Bachelor of Nursing.
Toni has significant experience, having worked in Brisbane’s Infectious Diseases ward before returning home to New Zealand, where she continued her career as a Clinical Nurse Specialist in Infection Prevention and Control within Te Whatu Ora (Health NZ).
Toni brings her expertise and dedication to our team, which is instrumental in providing top-tier infection prevention solutions to our clients.
Julie Hadfield
Accounts & Payroll
Julie is experienced in Accounts & Payroll Administration & after a long career in both the Financial & Local Government Sectors, is now working with our team. Julie brings her strong time management & organisational skills to our team, which is important to keep the company running in the background to enable the rest of our team to provide top notch service to all of our clients.
Julie is experienced in Accounts & Payroll Administration & after a long career in both the Financial & Local Government Sectors, is now working with our team. Julie brings her strong time management & organisational skills to our team, which is important to keep the company running in the background to enable the rest of our team to provide top notch service to all of our clients.
Andrea Murray
Content Editor
I attended Otago University in NZ and graduated as a Dental Surgeon. After 40 years in the profession, I retired in 2022. Infection prevention knowledge was part of everyday practice, dealing with sterilisation, hand hygiene, and cleaning.
Before retiring, I began doing some editing and proofreading for Bug Control as I am interested in the subject and in the English language. During the COVID-19 lockdown, I attended the ACIPC course "Introduction to Infection Prevention and Control", which increased my interest in the subject. I now work part-time as the Content Editor for the company.
I attended Otago University in NZ and graduated as a Dental Surgeon. After 40 years in the profession, I retired in 2022. Infection prevention knowledge was part of everyday practice, dealing with sterilisation, hand hygiene, and cleaning.
Before retiring, I began doing some editing and proofreading for Bug Control as I am interested in the subject and in the English language. During the COVID-19 lockdown, I attended the ACIPC course "Introduction to Infection Prevention and Control", which increased my interest in the subject. I now work part-time as the Content Editor for the company.
Personally, I lived in the UK for 10 years. My two children were born in Scotland, and now both are living in Europe, one in Amsterdam, Netherlands, and the other in Edinburgh, Scotland. I live close to Fairlie on the South Island of NZ, a beautiful part of the country, and I love being out of the city.
Princess
Customer Support
Princess began her career as a dedicated Customer Service Representative, honing her communication and problem-solving skills. She later transitioned into a Literary Specialist role, where she developed a keen eye for detail. Her journey then led her to a Sales Specialist position, where she excelled in client relations.
Now, as a Customer Support professional in Infection Prevention Services. Princess focuses on ensuring customer satisfaction, building loyalty, and enhancing the overall customer journey.
Princess began her career as a dedicated Customer Service Representative, honing her communication and problem-solving skills. She later transitioned into a Literary Specialist role, where she developed a keen eye for detail. Her journey then led her to a Sales Specialist position, where she excelled in client relations.
Now, as a Customer Support professional in Infection Prevention Services. Princess focuses on ensuring customer satisfaction, building loyalty, and enhancing the overall customer journey.
Dianne Newey
Senior Infection Prevention and Control Consultant
Dianne is a Senior Clinical Consultant at Infection Prevention Services (IPS), bringing over 35 years of nursing experience and a depth of clinical knowledge that most people would need two careers to accumulate.
Having served as Clinical Director at Royal Ryde Rehabilitation Hospital alongside a career spanning the full breadth of clinical practice, Dianne has seen it all — and more importantly, knows exactly what to do about it. She is the person in the room that everyone quietly hopes will speak first.
For more than seven years she has been a cornerstone of the IPS team, providing clinical advice, developing and reviewing policies and procedures, delivering monthly IPC webinars to IP Leads, and conducting environmental audits in aged care facilities across Australia and New Zealand. If infection prevention has a question, Dianne almost certainly has the answer — and she'll deliver it with a laugh that you'll hear from the other end of the corridor.
A true fountain of knowledge, wrapped in the kind of warmth and humour that only three decades of nursing can produce. Customers don't just trust Dianne — they look forward to hearing from her.
Dianne is a Senior Clinical Consultant at Infection Prevention Services (IPS), bringing over 35 years of nursing experience and a depth of clinical knowledge that most people would need two careers to accumulate.
Having served as Clinical Director at Royal Ryde Rehabilitation Hospital alongside a career spanning the full breadth of clinical practice, Dianne has seen it all — and more importantly, knows exactly what to do about it. She is the person in the room that everyone quietly hopes will speak first.
For more than seven years she has been a cornerstone of the IPS team, providing clinical advice, developing and reviewing policies and procedures, delivering monthly IPC webinars to IP Leads, and conducting environmental audits in aged care facilities across Australia and New Zealand. If infection prevention has a question, Dianne almost certainly has the answer — and she'll deliver it with a laugh that you'll hear from the other end of the corridor.
A true fountain of knowledge, wrapped in the kind of warmth and humour that only three decades of nursing can produce. Customers don't just trust Dianne — they look forward to hearing from her.
Caoimhe (Keva) Stewart
Clinical & Business Operations Manager
Caoimhe is the Clinical & Business Operations Manager at Infection Prevention Services (IPS), bringing a clinical background as a Registered Nurse across the UK and Australia — and an almost unsettling ability to make technology do exactly what she wants.
With experience in Occupational Health, Palliative Care, and Community Nursing, she understands the real challenges faced by healthcare teams. What she may lack in stature she more than makes up for in impact — Caoimhe is the kind of person who walks into a problem, sizes it up, and has three solutions before anyone else has finished reading the brief.
Customers love her. Not just because she delivers — though she always does — but because she genuinely cares about the outcome on the other side. She is passionate about creating seamless learning experiences and empowering organisations with the tools, knowledge, and support needed to strengthen infection prevention practices and improve care outcomes.
Small in size. Mighty in results. Completely irreplaceable.
Caoimhe is the Clinical & Business Operations Manager at Infection Prevention Services (IPS), bringing a clinical background as a Registered Nurse across the UK and Australia — and an almost unsettling ability to make technology do exactly what she wants.
With experience in Occupational Health, Palliative Care, and Community Nursing, she understands the real challenges faced by healthcare teams. What she may lack in stature she more than makes up for in impact — Caoimhe is the kind of person who walks into a problem, sizes it up, and has three solutions before anyone else has finished reading the brief.
Customers love her. Not just because she delivers — though she always does — but because she genuinely cares about the outcome on the other side. She is passionate about creating seamless learning experiences and empowering organisations with the tools, knowledge, and support needed to strengthen infection prevention practices and improve care outcomes.
Small in size. Mighty in results. Completely irreplaceable.
Bridgette Mackie
Clinical Nurse Educator
Bridgette is an experienced New Zealand Registered Nurse, qualified Healthcare Auditor, and Healthcare Educator with a strong background in clinical quality, competency assessment, and infection prevention. She has led large-scale OSCE and CAP training programmes for internationally qualified nurses, developed sector-specific educational resources, and coordinated HealthCERT audit preparation in the surgical sector.
Known for her engaging teaching style and genuine passion for supporting learners, Bridgette excels at making complex topics accessible and relevant. She blends operational leadership with a deep commitment to professional development and safe, effective practice.
Bridgette is an experienced New Zealand Registered Nurse, qualified Healthcare Auditor, and Healthcare Educator with a strong background in clinical quality, competency assessment, and infection prevention. She has led large-scale OSCE and CAP training programmes for internationally qualified nurses, developed sector-specific educational resources, and coordinated HealthCERT audit preparation in the surgical sector.
Known for her engaging teaching style and genuine passion for supporting learners, Bridgette excels at making complex topics accessible and relevant. She blends operational leadership with a deep commitment to professional development and safe, effective practice.

