Oct 22
Hydration and UTI Management
Introduction
As we enter summer, reports of UTIs increase. Hydration is a crucial factor that should
not be overlooked. This blog focuses on optimising hydration and managing urinary tract
infections (UTIs), particularly in aged care settings in Australia and New Zealand,
especially during warmer months. The text emphasises that dehydration is a significant
risk factor for UTIs and other serious health issues like delirium and heatstroke in older
adults. To address this, there are innovative, structured strategies to encourage
residents to meet their daily fluid targets, such as scheduling regular rounds and
incorporating fluid-rich foods. Importantly, the current national guidelines strongly
discourage the routine use of urine dipstick tests to diagnose UTIs, as these often result
in unnecessary antibiotic treatment of Asymptomatic Bacteriuria (ASB). Instead, best
practice suggests focusing on aggressive hydration, pain relief, and diagnosing UTIs
based solely on the presence of new or worsening clinical urinary symptoms.
We review best practice guidelines from Australia and New Zealand, highlighting innovative hydration approaches, the important shift away from outdated diagnostic tests, and effective non-antibiotic methods for managing UTIs. By implementing these evidence-based practices, we can enhance resident outcomes, minimise unnecessary antibiotic use, and promote antimicrobial stewardship.
We review best practice guidelines from Australia and New Zealand, highlighting innovative hydration approaches, the important shift away from outdated diagnostic tests, and effective non-antibiotic methods for managing UTIs. By implementing these evidence-based practices, we can enhance resident outcomes, minimise unnecessary antibiotic use, and promote antimicrobial stewardship.

Part 1: Mastering Resident Hydration
Hydration is essential for a healthy mind and body. For older adults, maintaining enough
f
luid intake is not just about comfort; it is vital in preventing a range of health issues.
Dehydration can have a serious impact on an older person's health, directly impairing
brain function and leading to critical medical events. Conversely, staying well-hydrated
can boost endurance, lower the heart rate, speed up recovery, and lift mood. Why are
residents in aged care so vulnerable to dehydration?
Adults can lose nearly 2.5 litres of water daily through normal activities, making regular
Adults can lose nearly 2.5 litres of water daily through normal activities, making regular
fluid intake essential. However, several factors specific to older adults render them
especially vulnerable.
- Reduced Thirst Sensation: It’s important to remember that when an older person feels thirsty, their body is already dehydrated. Their natural thirst response is less sensitive.
- Cognitive and Mobility Limitations: Residents with cognitive impairments like dementia may forget to drink, while those with mobility issues might be unable to get a drink themselves.
- Medication Side Effects: Common medications, like diuretics, can lead to increased fluid loss.
- Decreased Appetite and Activity: As appetite and physical activity often decline with age, so can the motivation and routine of drinking fluids.
- Poor Hydration Literacy: A 2017 study found that many older Australians lack
essential knowledge about hydration health literacy. They often overestimate the
amount of fluid loss required to cause symptoms and underestimate the amount of
fluid that needs to be replaced. Additionally, they may not recognise the signs of
dehydration in themselves.
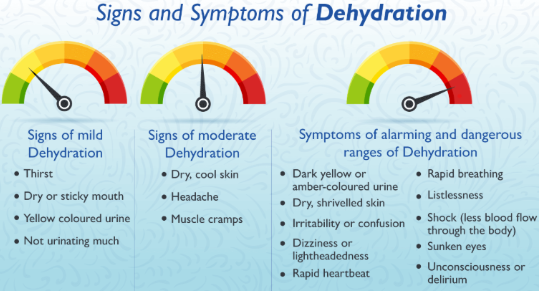
Recognising the Signs: From Mild to Severe
Early identification is essential. Care staff should remain alert for the common signs of
dehydration, which include:
- Fatigue or lethargy
- Muscle weakness and cramps
- Headaches and dizziness
- Nausea
- Forgetfulness and confusion
- Cracked lips and a dry or sticky mouth
- Low urination
- Sunken eyes
If left unchecked, dehydration can cause much more severe medical episodes, such as:
- Psychosis or delirium (dehydration being one of the most common causes of delirium)
- Urinary and kidney problems
- Heat injuries, including heat stroke Seizures
- Seizures
- Low blood volume shock (hypovolemic shock)
- In extreme cases, death
The Challenges of Hydration in Dementia Care
Residents living with dementia face an increased risk of dehydration. Water is crucial for
this group to help prevent behavioural changes, delirium, and depression. However,
specific challenges include:
- Forgetting to drink or even losing the ability to drink.
- Difficulty swallowing (dysphagia), which may lead to choking. A speech pathologist can help address these issues.
- Inability to express thirst or need for help because of loss of mobility or
communication skills
Practical and Creative Hydration Strategies
The aim for most residents is a daily fluid intake of at least 1.5 to 2.0 litres, unless they
are on a fluid restriction prescribed by a doctor. Moving beyond simply asking, "Would
you like a drink?" is essential. Here are evidence-based strategies to reach this target:
1. Make it Routine and Structured:
- Scheduled Hydration Rounds: Conduct rounds every 1.5 to 2 hours throughout the day. Use more assertive, structured prompts, such as "I'd like you to have a drink now."
- Routine Association: Link drinking fluids to other regular events, such as with all
medication rounds, before or after showering, after toileting, and during daily activities.
2. Think Beyond the Water Jug:
- Fluid-Rich Foods: A large part of fluid intake can come from food. Regularly offer high fluid options such as:
◦ Thin custard and yoghurt.
◦ Water-rich fruits and vegetables such as watermelon, cucumber, grapes, tomatoes, spinach and broccoli.

◦ Soups and broths, served at the resident's preferred temperature.
- Offer Variety: To encourage fluid intake, provide alternatives to plain water. This can
include cordials, fruit or vegetable juices, or non-caffeinated teas. Changing the
temperature can also help. While caffeinated drinks and alcohol should be limited as
they can cause dehydration, offering a preferred drink like tea or coffee is better than
letting the resident refuse fluids altogether.
3. Ensure Accessibility and Support
- Personalised Preferences: Find out what each resident truly enjoys drinking and make sure all staff are aware of this.
- Easy Access: Always make sure a drink is within easy reach of the resident.
- Assistive Aids: Use equipment such as extra-long straws, two-handled cups, or other
modified cups to help residents maintain their independence with drinking.
4. Monitor Carefully
- High-Risk Monitoring: For residents at high risk of dehydration (e.g., those with advanced dementia, on diuretics, or with a fever), use and accurately maintain fluid balance charts.
- Addressing Systemic Failures: The Royal Commission into Aged Care Quality and
Safety has highlighted that some facilities are not managing residents' fluid charts
properly. Meticulous charting is not just paperwork; it is a vital clinical tool for
preventing severe dehydration.
Part 2: A Modern Approach to UTI Diagnosis and Management
Urinary tract infections are a common concern in aged care, but our approach to
diagnosing and treating them must align with current best practices to prevent the
significant harms of over-treatment.
The Verdict on Urine Dipsticks
This marks a crucial change in aged care practice. Clinical pathways at the national and
state levels in Australia and New Zealand strongly advocate against routinely using
urine dipstick tests for suspected UTIs in aged care residents.

The clear message is: Do NOT use a urine dipstick test to diagnose a UTI in an aged care
resident.
Why is this so critical? The reason lies in a condition called Asymptomatic Bacteriuria (ASB).
Why is this so critical? The reason lies in a condition called Asymptomatic Bacteriuria (ASB).
- What is ASB? ASB is the presence of bacteria in the urine without any clinical symptoms of infection. It is a normal, harmless colonisation of bacteria that does not require antibiotic treatment.
- How common is it? ASB is very prevalent among older adults. Up to 50% of older women and a notable number of older men experience it.
- The Dipstick Problem: A positive dipstick result (showing nitrites or leukocyte esterase) cannot differentiate between a genuine, symptomatic UTI and harmless ASB. This often results in the misdiagnosis and unnecessary treatment of ASB.
Treating ASB exposes residents to unnecessary antibiotics, increasing their risk of Clostridioides difficile infection and worsening the antimicrobial resistance (AMR) public health crisis. Additionally, treating ASB does not prevent future symptomatic UTIs and often causes more harm than good.
Best Practice: Clinical Assessment is Key
The focus should move from pursuing a positive test result to performing a
comprehensive clinical assessment. A suspected UTI diagnosis must rely on new or
worsening localised urinary symptoms.
Symptoms that may indicate a UTI:
- Cloudy or foul-smelling urine
- Burning or pain during urination (dysuria)
- New or worsening urinary frequency
- New or worsening urinary urgency
- Pain above the pubic bone (suprapubic pain)
- Newly onset incontinence
Symptoms that are NOT sufficient for a UTI diagnosis:
- A shift in behaviour
- A fall
- A general decline in condition
- Cloudy or foul-smelling urine
These vague symptoms are usually caused by other issues, with dehydration being a common cause. Cloudy or foul-smelling urine is most often a sign of dehydration or a reaction to certain foods or medications, not an infection.
Effective Management: Hydration and Non-Antibiotic Strategies First
Before prescribing an antibiotic, especially in mild cases or when symptoms are vague,
concentrate on these important non-pharmacological interventions:
1. Aggressive Hydration: This is the crucial first step. Addressing dehydration can often relieve mild urinary symptoms, such as painful urination (dysuria), and may be the only treatment needed to resolve the resident's condition.
2. Symptom and Pain Relief: Relieve discomfort with simple analgesics like paracetamol (if suitable for the resident). Urinary alkalisers can also help in easing symptoms, although they do not treat the underlying infection.
3. Perineal Hygiene: Practice regular and correct perineal cleaning, especially after toileting and incontinence episodes, to lower the bacterial load locally.
4. Topical Oestrogen: For postmenopausal women experiencing recurrent UTIs, intravaginal oestrogen (available as a cream or pessary) can be highly effective. It works by restoring healthy vaginal flora, which considerably reduces the occurrence of UTIs.
5. Catheter Management: For residents with an indwelling catheter, strict adherence to catheter care bundles is essential. If a UTI is suspected clinically, the catheter should ideally be removed or replaced before collecting a urine sample for culture (MC&S) to prevent contamination.

Conclusion: A Commitment to Better Care
Managing hydration and UTIs effectively in the summer months doesn't have to mean an
automatic spike in antibiotic prescribing. By rigorously prioritising hydration, avoiding
routine dipstick testing, and ensuring all diagnostic decisions are based on strong
clinical assessment and current national guidelines, we can greatly enhance the quality
of life for our residents. This approach not only delivers better, safer care but also
positions our facilities as leaders in antimicrobial stewardship.
Read more of our blogs, available on the HUB, the IPS website.
For individual questions, ask EVE for the answer to a clinical question and receive a
For individual questions, ask EVE for the answer to a clinical question and receive a
reply in your own language! Alternatively, our friendly team are available for enquiries at support@infectionprevention.care
We are on Facebook and LinkedIn. Follow us, like and share
Take advantage of our expertise in IPC. See the HUB for policies, resources and courses relating to this very important subject. Ask EVE for a quick answer to your question.
We are on Facebook and LinkedIn. Follow us, like and share
Take advantage of our expertise in IPC. See the HUB for policies, resources and courses relating to this very important subject. Ask EVE for a quick answer to your question.
Lyndon Forrest
Managing Director | CEO
Lyndon is the Managing Director of Infection Prevention Services (IPS), bringing over 30 years' experience supporting aged care providers across Australia and New Zealand.
With a background spanning outbreak response, compliance, and infection risk management — alongside hands-on experience leading teams, managing multi-site operations, and navigating business turnaround — he understands both the clinical and organisational pressures aged care providers face. Lyndon holds a Master of Commerce (Industrial Relations), and applies that foundation to the people, process, and growth challenges that come with running a complex healthcare services business.
He is passionate about building the systems and capability that make infection prevention sustainable — not just compliant — and about helping organisations grow their confidence alongside their practice.
Lyndon's focus is straightforward: strengthen operations, develop the right people, and drive proactive infection prevention strategies that protect residents, staff, and communities for the long term.
Lyndon is the Managing Director of Infection Prevention Services (IPS), bringing over 30 years' experience supporting aged care providers across Australia and New Zealand.
With a background spanning outbreak response, compliance, and infection risk management — alongside hands-on experience leading teams, managing multi-site operations, and navigating business turnaround — he understands both the clinical and organisational pressures aged care providers face. Lyndon holds a Master of Commerce (Industrial Relations), and applies that foundation to the people, process, and growth challenges that come with running a complex healthcare services business.
He is passionate about building the systems and capability that make infection prevention sustainable — not just compliant — and about helping organisations grow their confidence alongside their practice.
Lyndon's focus is straightforward: strengthen operations, develop the right people, and drive proactive infection prevention strategies that protect residents, staff, and communities for the long term.
Erica Callaghan
Marketing Manager
Erica Callaghan is a dedicated professional with a rich background in agriculture and nutrient management. Growing up on her family's farm in Mid Canterbury, she developed a deep passion for farming. She currently resides on her partner's arable property in South Canterbury.
In 2017, Erica joined the Farm Sustainability team, focusing on nutrient management and environmental stewardship. In February 2024, she became the Manager of Marketing and Sales at Bug Control New Zealand - Infection Prevention Services, where her passion now includes improving infection prevention outcomes.
Outside of work, Erica loves cooking and traveling, often combining her culinary interests with her explorations in Italy and Vietnam. She enjoys entertaining family and friends and remains actively involved in farm activities, especially during harvest season.
Erica Callaghan is a dedicated professional with a rich background in agriculture and nutrient management. Growing up on her family's farm in Mid Canterbury, she developed a deep passion for farming. She currently resides on her partner's arable property in South Canterbury.
In 2017, Erica joined the Farm Sustainability team, focusing on nutrient management and environmental stewardship. In February 2024, she became the Manager of Marketing and Sales at Bug Control New Zealand - Infection Prevention Services, where her passion now includes improving infection prevention outcomes.
Outside of work, Erica loves cooking and traveling, often combining her culinary interests with her explorations in Italy and Vietnam. She enjoys entertaining family and friends and remains actively involved in farm activities, especially during harvest season.
Toni Sherriff
Clinical Nurse Specialist
Toni is a Registered Nurse with extensive experience in Infection Prevention and Control. Her career began as a kitchen hand and caregiver in Aged Care facilities, followed by earning a Bachelor of Nursing.
Toni has significant experience, having worked in Brisbane’s Infectious Diseases ward before returning home to New Zealand, where she continued her career as a Clinical Nurse Specialist in Infection Prevention and Control within Te Whatu Ora (Health NZ).
Toni brings her expertise and dedication to our team, which is instrumental in providing top-tier infection prevention solutions to our clients.
Toni is a Registered Nurse with extensive experience in Infection Prevention and Control. Her career began as a kitchen hand and caregiver in Aged Care facilities, followed by earning a Bachelor of Nursing.
Toni has significant experience, having worked in Brisbane’s Infectious Diseases ward before returning home to New Zealand, where she continued her career as a Clinical Nurse Specialist in Infection Prevention and Control within Te Whatu Ora (Health NZ).
Toni brings her expertise and dedication to our team, which is instrumental in providing top-tier infection prevention solutions to our clients.
Julie Hadfield
Accounts & Payroll
Julie is experienced in Accounts & Payroll Administration & after a long career in both the Financial & Local Government Sectors, is now working with our team. Julie brings her strong time management & organisational skills to our team, which is important to keep the company running in the background to enable the rest of our team to provide top notch service to all of our clients.
Julie is experienced in Accounts & Payroll Administration & after a long career in both the Financial & Local Government Sectors, is now working with our team. Julie brings her strong time management & organisational skills to our team, which is important to keep the company running in the background to enable the rest of our team to provide top notch service to all of our clients.
Andrea Murray
Content Editor
I attended Otago University in NZ and graduated as a Dental Surgeon. After 40 years in the profession, I retired in 2022. Infection prevention knowledge was part of everyday practice, dealing with sterilisation, hand hygiene, and cleaning.
Before retiring, I began doing some editing and proofreading for Bug Control as I am interested in the subject and in the English language. During the COVID-19 lockdown, I attended the ACIPC course "Introduction to Infection Prevention and Control", which increased my interest in the subject. I now work part-time as the Content Editor for the company.
I attended Otago University in NZ and graduated as a Dental Surgeon. After 40 years in the profession, I retired in 2022. Infection prevention knowledge was part of everyday practice, dealing with sterilisation, hand hygiene, and cleaning.
Before retiring, I began doing some editing and proofreading for Bug Control as I am interested in the subject and in the English language. During the COVID-19 lockdown, I attended the ACIPC course "Introduction to Infection Prevention and Control", which increased my interest in the subject. I now work part-time as the Content Editor for the company.
Personally, I lived in the UK for 10 years. My two children were born in Scotland, and now both are living in Europe, one in Amsterdam, Netherlands, and the other in Edinburgh, Scotland. I live close to Fairlie on the South Island of NZ, a beautiful part of the country, and I love being out of the city.
Princess
Customer Support
Princess began her career as a dedicated Customer Service Representative, honing her communication and problem-solving skills. She later transitioned into a Literary Specialist role, where she developed a keen eye for detail. Her journey then led her to a Sales Specialist position, where she excelled in client relations.
Now, as a Customer Support professional in Infection Prevention Services. Princess focuses on ensuring customer satisfaction, building loyalty, and enhancing the overall customer journey.
Princess began her career as a dedicated Customer Service Representative, honing her communication and problem-solving skills. She later transitioned into a Literary Specialist role, where she developed a keen eye for detail. Her journey then led her to a Sales Specialist position, where she excelled in client relations.
Now, as a Customer Support professional in Infection Prevention Services. Princess focuses on ensuring customer satisfaction, building loyalty, and enhancing the overall customer journey.
Dianne Newey
Senior Infection Prevention and Control Consultant
Dianne is a Senior Clinical Consultant at Infection Prevention Services (IPS), bringing over 35 years of nursing experience and a depth of clinical knowledge that most people would need two careers to accumulate.
Having served as Clinical Director at Royal Ryde Rehabilitation Hospital alongside a career spanning the full breadth of clinical practice, Dianne has seen it all — and more importantly, knows exactly what to do about it. She is the person in the room that everyone quietly hopes will speak first.
For more than seven years she has been a cornerstone of the IPS team, providing clinical advice, developing and reviewing policies and procedures, delivering monthly IPC webinars to IP Leads, and conducting environmental audits in aged care facilities across Australia and New Zealand. If infection prevention has a question, Dianne almost certainly has the answer — and she'll deliver it with a laugh that you'll hear from the other end of the corridor.
A true fountain of knowledge, wrapped in the kind of warmth and humour that only three decades of nursing can produce. Customers don't just trust Dianne — they look forward to hearing from her.
Dianne is a Senior Clinical Consultant at Infection Prevention Services (IPS), bringing over 35 years of nursing experience and a depth of clinical knowledge that most people would need two careers to accumulate.
Having served as Clinical Director at Royal Ryde Rehabilitation Hospital alongside a career spanning the full breadth of clinical practice, Dianne has seen it all — and more importantly, knows exactly what to do about it. She is the person in the room that everyone quietly hopes will speak first.
For more than seven years she has been a cornerstone of the IPS team, providing clinical advice, developing and reviewing policies and procedures, delivering monthly IPC webinars to IP Leads, and conducting environmental audits in aged care facilities across Australia and New Zealand. If infection prevention has a question, Dianne almost certainly has the answer — and she'll deliver it with a laugh that you'll hear from the other end of the corridor.
A true fountain of knowledge, wrapped in the kind of warmth and humour that only three decades of nursing can produce. Customers don't just trust Dianne — they look forward to hearing from her.
Caoimhe (Keva) Stewart
Clinical & Business Operations Manager
Caoimhe is the Clinical & Business Operations Manager at Infection Prevention Services (IPS), bringing a clinical background as a Registered Nurse across the UK and Australia — and an almost unsettling ability to make technology do exactly what she wants.
With experience in Occupational Health, Palliative Care, and Community Nursing, she understands the real challenges faced by healthcare teams. What she may lack in stature she more than makes up for in impact — Caoimhe is the kind of person who walks into a problem, sizes it up, and has three solutions before anyone else has finished reading the brief.
Customers love her. Not just because she delivers — though she always does — but because she genuinely cares about the outcome on the other side. She is passionate about creating seamless learning experiences and empowering organisations with the tools, knowledge, and support needed to strengthen infection prevention practices and improve care outcomes.
Small in size. Mighty in results. Completely irreplaceable.
Caoimhe is the Clinical & Business Operations Manager at Infection Prevention Services (IPS), bringing a clinical background as a Registered Nurse across the UK and Australia — and an almost unsettling ability to make technology do exactly what she wants.
With experience in Occupational Health, Palliative Care, and Community Nursing, she understands the real challenges faced by healthcare teams. What she may lack in stature she more than makes up for in impact — Caoimhe is the kind of person who walks into a problem, sizes it up, and has three solutions before anyone else has finished reading the brief.
Customers love her. Not just because she delivers — though she always does — but because she genuinely cares about the outcome on the other side. She is passionate about creating seamless learning experiences and empowering organisations with the tools, knowledge, and support needed to strengthen infection prevention practices and improve care outcomes.
Small in size. Mighty in results. Completely irreplaceable.
Bridgette Mackie
Clinical Nurse Educator
Bridgette is an experienced New Zealand Registered Nurse, qualified Healthcare Auditor, and Healthcare Educator with a strong background in clinical quality, competency assessment, and infection prevention. She has led large-scale OSCE and CAP training programmes for internationally qualified nurses, developed sector-specific educational resources, and coordinated HealthCERT audit preparation in the surgical sector.
Known for her engaging teaching style and genuine passion for supporting learners, Bridgette excels at making complex topics accessible and relevant. She blends operational leadership with a deep commitment to professional development and safe, effective practice.
Bridgette is an experienced New Zealand Registered Nurse, qualified Healthcare Auditor, and Healthcare Educator with a strong background in clinical quality, competency assessment, and infection prevention. She has led large-scale OSCE and CAP training programmes for internationally qualified nurses, developed sector-specific educational resources, and coordinated HealthCERT audit preparation in the surgical sector.
Known for her engaging teaching style and genuine passion for supporting learners, Bridgette excels at making complex topics accessible and relevant. She blends operational leadership with a deep commitment to professional development and safe, effective practice.

