Apr 7
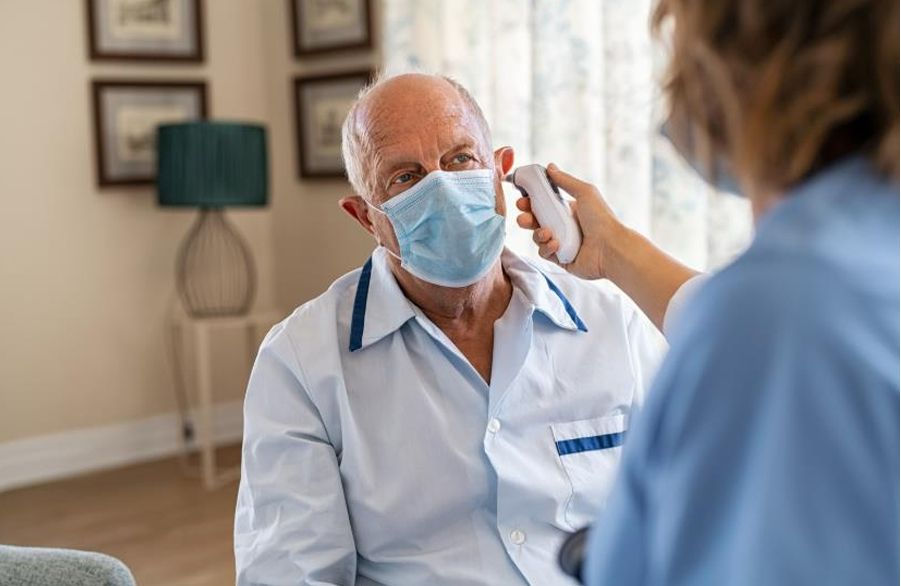
Keeping Residents Safe and Connected
Top Tips for the Winter Season
As we approach the 2026 winter season, our focus is on safeguarding our community
from respiratory illnesses such as influenza, RSV, and COVID-19. Balancing clinical
safety with the social well-being of our residents requires teamwork. By adopting these
practical strategies, we can create a warm, sociable environment while ensuring our
residents stay safe.
Vaccination remains our most effective shield against severe respiratory illness. Maintaining high vaccination rates, aiming for around 80% among staff, helps develop herd immunity within the facility. For residents, staying up to date with the 2026 vaccination schedule reduces the risk of hospitalisation and the severity of infection, ensuring compliance with standards and guidelines.
Vaccination remains our most effective shield against severe respiratory illness. Maintaining high vaccination rates, aiming for around 80% among staff, helps develop herd immunity within the facility. For residents, staying up to date with the 2026 vaccination schedule reduces the risk of hospitalisation and the severity of infection, ensuring compliance with standards and guidelines.
1. Optimise Environmental Ventilation
Viruses flourish in stagnant indoor air, particularly when windows remain closed during
colder weather.
- "Gentle Ventilation": Periodically crack windows in communal areas for 10–15 minutes when residents are not around, such as during cleaning, to refresh the air.
- HEPA Purifiers: Make sure HEPA units are plugged in, switched on, and placed in busy areas like dining rooms to constantly "scrub" viral particles from the air.
- Temperature Balance: Keep an eye on the facility to ensure the temperature is
comfortable while allowing for necessary air exchange.
2. Implement Resident-Centric Hand Hygiene
Although staff hygiene is the gold standard, residents often touch shared surfaces such
as handrails and tabletops.
- Point-of-Care Access: Place alcohol-based hand rub (ABHR) at dining room entrances and activity stations within residents’ reach, and at each resident’s bedside.
- Social "Moments": Encourage residents to do hand hygiene together before meals or group gatherings to support those with mobility or cognitive challenges.
- Proactive Assistance: Promptly help residents with hand hygiene immediately
after group activities to prevent the spread of infection.
3. Use Risk-Based PPE & Smart Masking
PPE should be used thoughtfully to prevent social isolation, particularly for our most
vulnerable residents.
- Community Peaks: Advise staff and visitors to wear masks during times of high community transmission, even if there is no active outbreak.
- Clear Communication: Use transparent masks for residents with hearing loss or
cognitive decline to enable lip-reading, facial cues, and improved emotional
connection.

- Waste Management: Regularly empty waste bins for used masks and tissues to
prevent overflow.
4. Leverage "Partners in Care"
Families and close friends are vital for mental health, but they must be educated to
become "safe visitors".
- Formal Designation: Treat these contacts as "Partners in Care" by providing them with basic infection control training.
- Symptom Vigilance: Remind visitors to stay home if they have even a "minor" symptom of infection, such as a scratchy throat, cough, or fatigue.
- Pre-Visit Testing: Encourage visitors to perform a 4 in 1 Rapid Antigen Test (RAT)
(these test for COVID-19/RSV/Influenza A&B), before arrival especially when
community risk is high.
5. Prioritise Respiratory Etiquette
Consistent practice throughout the facility prevents droplets from remaining on
surfaces.
- Cough Stations: Have tissues, hand sanitiser and foot pedal bins in common areas, such as dining rooms, lounge rooms and activity areas.
- "Catch it, Bin it, Kill it": Use age-appropriate, high-contrast visual posters to
remind residents and contractors of proper respiratory etiquette.
6. 2026 Vaccination Compliance & Tracking
To satisfy clinical governance standards, we must proactively organise and monitor all
vaccinations within the facility
- Resident Schedule: Ensure residents aged 75 and over receive a COVID-19 dose every 6 months, while those aged 65–74 get theirs every 12 months.
- Annual Milestones: All residents should receive their 2026 flu vaccination by 30 April, with mandatory data submission due by 31 July into AIR.
- Audit the immunisation history of every new resident within 48 hours of admission.
- System Triggers: Use tracking software to flag "Red Flags," such as residents who
are 5 months post-vaccination, to facilitate a 14-day planning window for their
next dose.
Conclusion
Building a strong "safety culture" involves looking out for each other. If you see a
colleague miss a hand hygiene moment or find a sanitiser dispenser empty, please
speak up. By incorporating these clinical safeguards into our daily routines, we protect
our residents' health while respecting their need for a vibrant personal and social life.
For more information on this subject, and many others, visit the HUB or ask EVE for an answer to that tricky question. More blogs are also available to read on the HUB
For more information on this subject, and many others, visit the HUB or ask EVE for an answer to that tricky question. More blogs are also available to read on the HUB
Visit the HUB for further information from our trusted resources and previous blog
posts.
Ask EVE if you have a specific question – she has access to these resources.
Contact our team at support@infectiontionprevention.care
We are on Facebook and LinkedIn – be sure to like and share
Take advantage of our expertise in IPC. See the HUB for policies, resources and courses relating to this very important subject. Ask EVE for a quick answer to your question.
Ask EVE if you have a specific question – she has access to these resources.
Contact our team at support@infectiontionprevention.care
We are on Facebook and LinkedIn – be sure to like and share
Take advantage of our expertise in IPC. See the HUB for policies, resources and courses relating to this very important subject. Ask EVE for a quick answer to your question.
Lyndon Forrest
Managing Director | CEO
Lyndon is the Managing Director of Infection Prevention Services (IPS), bringing over 30 years' experience supporting aged care providers across Australia and New Zealand.
With a background spanning outbreak response, compliance, and infection risk management — alongside hands-on experience leading teams, managing multi-site operations, and navigating business turnaround — he understands both the clinical and organisational pressures aged care providers face. Lyndon holds a Master of Commerce (Industrial Relations), and applies that foundation to the people, process, and growth challenges that come with running a complex healthcare services business.
He is passionate about building the systems and capability that make infection prevention sustainable — not just compliant — and about helping organisations grow their confidence alongside their practice.
Lyndon's focus is straightforward: strengthen operations, develop the right people, and drive proactive infection prevention strategies that protect residents, staff, and communities for the long term.
Lyndon is the Managing Director of Infection Prevention Services (IPS), bringing over 30 years' experience supporting aged care providers across Australia and New Zealand.
With a background spanning outbreak response, compliance, and infection risk management — alongside hands-on experience leading teams, managing multi-site operations, and navigating business turnaround — he understands both the clinical and organisational pressures aged care providers face. Lyndon holds a Master of Commerce (Industrial Relations), and applies that foundation to the people, process, and growth challenges that come with running a complex healthcare services business.
He is passionate about building the systems and capability that make infection prevention sustainable — not just compliant — and about helping organisations grow their confidence alongside their practice.
Lyndon's focus is straightforward: strengthen operations, develop the right people, and drive proactive infection prevention strategies that protect residents, staff, and communities for the long term.
Erica Callaghan
Marketing Manager
Erica Callaghan is a dedicated professional with a rich background in agriculture and nutrient management. Growing up on her family's farm in Mid Canterbury, she developed a deep passion for farming. She currently resides on her partner's arable property in South Canterbury.
In 2017, Erica joined the Farm Sustainability team, focusing on nutrient management and environmental stewardship. In February 2024, she became the Manager of Marketing and Sales at Bug Control New Zealand - Infection Prevention Services, where her passion now includes improving infection prevention outcomes.
Outside of work, Erica loves cooking and traveling, often combining her culinary interests with her explorations in Italy and Vietnam. She enjoys entertaining family and friends and remains actively involved in farm activities, especially during harvest season.
Erica Callaghan is a dedicated professional with a rich background in agriculture and nutrient management. Growing up on her family's farm in Mid Canterbury, she developed a deep passion for farming. She currently resides on her partner's arable property in South Canterbury.
In 2017, Erica joined the Farm Sustainability team, focusing on nutrient management and environmental stewardship. In February 2024, she became the Manager of Marketing and Sales at Bug Control New Zealand - Infection Prevention Services, where her passion now includes improving infection prevention outcomes.
Outside of work, Erica loves cooking and traveling, often combining her culinary interests with her explorations in Italy and Vietnam. She enjoys entertaining family and friends and remains actively involved in farm activities, especially during harvest season.
Toni Sherriff
Clinical Nurse Specialist
Toni is a Registered Nurse with extensive experience in Infection Prevention and Control. Her career began as a kitchen hand and caregiver in Aged Care facilities, followed by earning a Bachelor of Nursing.
Toni has significant experience, having worked in Brisbane’s Infectious Diseases ward before returning home to New Zealand, where she continued her career as a Clinical Nurse Specialist in Infection Prevention and Control within Te Whatu Ora (Health NZ).
Toni brings her expertise and dedication to our team, which is instrumental in providing top-tier infection prevention solutions to our clients.
Toni is a Registered Nurse with extensive experience in Infection Prevention and Control. Her career began as a kitchen hand and caregiver in Aged Care facilities, followed by earning a Bachelor of Nursing.
Toni has significant experience, having worked in Brisbane’s Infectious Diseases ward before returning home to New Zealand, where she continued her career as a Clinical Nurse Specialist in Infection Prevention and Control within Te Whatu Ora (Health NZ).
Toni brings her expertise and dedication to our team, which is instrumental in providing top-tier infection prevention solutions to our clients.
Julie Hadfield
Accounts & Payroll
Julie is experienced in Accounts & Payroll Administration & after a long career in both the Financial & Local Government Sectors, is now working with our team. Julie brings her strong time management & organisational skills to our team, which is important to keep the company running in the background to enable the rest of our team to provide top notch service to all of our clients.
Julie is experienced in Accounts & Payroll Administration & after a long career in both the Financial & Local Government Sectors, is now working with our team. Julie brings her strong time management & organisational skills to our team, which is important to keep the company running in the background to enable the rest of our team to provide top notch service to all of our clients.
Andrea Murray
Content Editor
I attended Otago University in NZ and graduated as a Dental Surgeon. After 40 years in the profession, I retired in 2022. Infection prevention knowledge was part of everyday practice, dealing with sterilisation, hand hygiene, and cleaning.
Before retiring, I began doing some editing and proofreading for Bug Control as I am interested in the subject and in the English language. During the COVID-19 lockdown, I attended the ACIPC course "Introduction to Infection Prevention and Control", which increased my interest in the subject. I now work part-time as the Content Editor for the company.
I attended Otago University in NZ and graduated as a Dental Surgeon. After 40 years in the profession, I retired in 2022. Infection prevention knowledge was part of everyday practice, dealing with sterilisation, hand hygiene, and cleaning.
Before retiring, I began doing some editing and proofreading for Bug Control as I am interested in the subject and in the English language. During the COVID-19 lockdown, I attended the ACIPC course "Introduction to Infection Prevention and Control", which increased my interest in the subject. I now work part-time as the Content Editor for the company.
Personally, I lived in the UK for 10 years. My two children were born in Scotland, and now both are living in Europe, one in Amsterdam, Netherlands, and the other in Edinburgh, Scotland. I live close to Fairlie on the South Island of NZ, a beautiful part of the country, and I love being out of the city.
Princess
Customer Support
Princess began her career as a dedicated Customer Service Representative, honing her communication and problem-solving skills. She later transitioned into a Literary Specialist role, where she developed a keen eye for detail. Her journey then led her to a Sales Specialist position, where she excelled in client relations.
Now, as a Customer Support professional in Infection Prevention Services. Princess focuses on ensuring customer satisfaction, building loyalty, and enhancing the overall customer journey.
Princess began her career as a dedicated Customer Service Representative, honing her communication and problem-solving skills. She later transitioned into a Literary Specialist role, where she developed a keen eye for detail. Her journey then led her to a Sales Specialist position, where she excelled in client relations.
Now, as a Customer Support professional in Infection Prevention Services. Princess focuses on ensuring customer satisfaction, building loyalty, and enhancing the overall customer journey.
Dianne Newey
Senior Infection Prevention and Control Consultant
Dianne is a Senior Clinical Consultant at Infection Prevention Services (IPS), bringing over 35 years of nursing experience and a depth of clinical knowledge that most people would need two careers to accumulate.
Having served as Clinical Director at Royal Ryde Rehabilitation Hospital alongside a career spanning the full breadth of clinical practice, Dianne has seen it all — and more importantly, knows exactly what to do about it. She is the person in the room that everyone quietly hopes will speak first.
For more than seven years she has been a cornerstone of the IPS team, providing clinical advice, developing and reviewing policies and procedures, delivering monthly IPC webinars to IP Leads, and conducting environmental audits in aged care facilities across Australia and New Zealand. If infection prevention has a question, Dianne almost certainly has the answer — and she'll deliver it with a laugh that you'll hear from the other end of the corridor.
A true fountain of knowledge, wrapped in the kind of warmth and humour that only three decades of nursing can produce. Customers don't just trust Dianne — they look forward to hearing from her.
Dianne is a Senior Clinical Consultant at Infection Prevention Services (IPS), bringing over 35 years of nursing experience and a depth of clinical knowledge that most people would need two careers to accumulate.
Having served as Clinical Director at Royal Ryde Rehabilitation Hospital alongside a career spanning the full breadth of clinical practice, Dianne has seen it all — and more importantly, knows exactly what to do about it. She is the person in the room that everyone quietly hopes will speak first.
For more than seven years she has been a cornerstone of the IPS team, providing clinical advice, developing and reviewing policies and procedures, delivering monthly IPC webinars to IP Leads, and conducting environmental audits in aged care facilities across Australia and New Zealand. If infection prevention has a question, Dianne almost certainly has the answer — and she'll deliver it with a laugh that you'll hear from the other end of the corridor.
A true fountain of knowledge, wrapped in the kind of warmth and humour that only three decades of nursing can produce. Customers don't just trust Dianne — they look forward to hearing from her.
Caoimhe (Keva) Stewart
Clinical & Business Operations Manager
Caoimhe is the Clinical & Business Operations Manager at Infection Prevention Services (IPS), bringing a clinical background as a Registered Nurse across the UK and Australia — and an almost unsettling ability to make technology do exactly what she wants.
With experience in Occupational Health, Palliative Care, and Community Nursing, she understands the real challenges faced by healthcare teams. What she may lack in stature she more than makes up for in impact — Caoimhe is the kind of person who walks into a problem, sizes it up, and has three solutions before anyone else has finished reading the brief.
Customers love her. Not just because she delivers — though she always does — but because she genuinely cares about the outcome on the other side. She is passionate about creating seamless learning experiences and empowering organisations with the tools, knowledge, and support needed to strengthen infection prevention practices and improve care outcomes.
Small in size. Mighty in results. Completely irreplaceable.
Caoimhe is the Clinical & Business Operations Manager at Infection Prevention Services (IPS), bringing a clinical background as a Registered Nurse across the UK and Australia — and an almost unsettling ability to make technology do exactly what she wants.
With experience in Occupational Health, Palliative Care, and Community Nursing, she understands the real challenges faced by healthcare teams. What she may lack in stature she more than makes up for in impact — Caoimhe is the kind of person who walks into a problem, sizes it up, and has three solutions before anyone else has finished reading the brief.
Customers love her. Not just because she delivers — though she always does — but because she genuinely cares about the outcome on the other side. She is passionate about creating seamless learning experiences and empowering organisations with the tools, knowledge, and support needed to strengthen infection prevention practices and improve care outcomes.
Small in size. Mighty in results. Completely irreplaceable.
Bridgette Mackie
Clinical Nurse Educator
Bridgette is an experienced New Zealand Registered Nurse, qualified Healthcare Auditor, and Healthcare Educator with a strong background in clinical quality, competency assessment, and infection prevention. She has led large-scale OSCE and CAP training programmes for internationally qualified nurses, developed sector-specific educational resources, and coordinated HealthCERT audit preparation in the surgical sector.
Known for her engaging teaching style and genuine passion for supporting learners, Bridgette excels at making complex topics accessible and relevant. She blends operational leadership with a deep commitment to professional development and safe, effective practice.
Bridgette is an experienced New Zealand Registered Nurse, qualified Healthcare Auditor, and Healthcare Educator with a strong background in clinical quality, competency assessment, and infection prevention. She has led large-scale OSCE and CAP training programmes for internationally qualified nurses, developed sector-specific educational resources, and coordinated HealthCERT audit preparation in the surgical sector.
Known for her engaging teaching style and genuine passion for supporting learners, Bridgette excels at making complex topics accessible and relevant. She blends operational leadership with a deep commitment to professional development and safe, effective practice.

